Assisted living provides personal care services and daily living assistance for seniors who remain largely independent, whereas memory care offers specialized dementia care programs with secured environments, behavioral support, and trained staff specifically for individuals with Alzheimer’s disease, dementia, or significant cognitive impairment. According to the Alzheimer’s Association (2024), memory care facilities typically cost 20-30% more than assisted living communities due to specialized training requirements, enhanced safety features, and lower staff-to-resident ratios.
Quick Comparison: Assisted Living vs Memory Care
| Feature | Assisted Living | Memory Care |
|---|---|---|
| Primary Purpose | Daily living assistance for independent seniors | Cognitive support services and dementia-specific care |
| Security Level | Standard monitoring systems | Secured memory care units with wandering prevention |
| Staff Training | General caregiving and Activities of Daily Living (ADLs) | Specialized dementia training and behavioral support |
| Staff-to-Resident Ratio | 1:8 to 1:15 | 1:4 to 1:8 |
| Average Monthly Cost (2025) | $4,500-$6,500 | $6,000-$9,000 |
| Environment Design | Standard residential care layout | Dementia-friendly with color-coded hallways and exit monitoring |
| Medical Support | Medication administration and basic healthcare services | Around-the-clock supervision with psychiatric care availability |
| Eligibility Criteria | Needs help with 2+ ADLs | Diagnosed cognitive impairment or moderate dementia |
What Is Assisted Living and Who Needs It?

Assisted living facilities provide residential care for seniors who require help with bathing assistance, dressing assistance, meal preparation, and housekeeping services but do not need skilled nursing care. According to the National Center for Assisted Living (2024), approximately 810,000 Americans reside in assisted living communities.
These senior living facilities offer a combination of independent living with supportive services. Certified nursing assistants help residents with personal care needs while encouraging maximum independence. Typical services include transportation services, social activities, and medication management.
Residents generally maintain their own apartments within the care facility. Unlike nursing homes, assisted living communities focus on maintaining resident autonomy while providing safety nets. The continuum of care model allows residents to age in place as needs evolve.
Services Provided in Assisted Living Communities
- Personal care services: Help with grooming, bathing, and dressing
- Medication administration: Supervised by licensed practical nurses
- Meal preparation: Three nutritious meals daily in communal dining
- Housekeeping services: Laundry and apartment cleaning
- Transportation services: Medical appointments and shopping trips
- Social activities: Exercise classes, outings, and entertainment programs
- Emergency response systems: 24-hour call buttons in each unit
What Is Memory Care and When Is It Necessary?
Memory care facilities are specialized dementia care centers designed exclusively for individuals with Alzheimer’s disease, vascular dementia, Lewy body dementia, frontotemporal dementia, or other neurological disorders causing memory loss. According to Johns Hopkins Medicine (2024), one in three seniors dies with Alzheimer’s disease or another dementia.
Unlike standard assisted living services, memory care units feature secured environments preventing residents from wandering unsupervised. Staff members receive specialized training in managing behavioral changes, sundowning, and the progression of dementia stages. The structured environment reduces confusion through consistent routines and therapeutic activities.
Memory support communities employ person-centered care approaches tailored to each resident’s cognitive abilities. Environmental design incorporates brain health principles with natural lighting, circular walking paths, and memory boxes outside rooms for orientation.
Distinguishing Features of Memory Care Units
- Secure facilities: Locked memory care units with alarmed exits
- Specialized caregivers: Dementia education and behavioral management training
- Cognitive rehabilitation: Memory-enhancing activities and sensory stimulation
- Safe living space: Obstacle-free layouts reducing fall prevention risks
- Continuous monitoring: Visual supervision throughout common areas
- Structured routines: Predictable daily schedules reducing anxiety
- Therapeutic activities: Music therapy, reminiscence therapy, and art programs
How Do Care Services Differ Between Assisted Living and Memory Care?
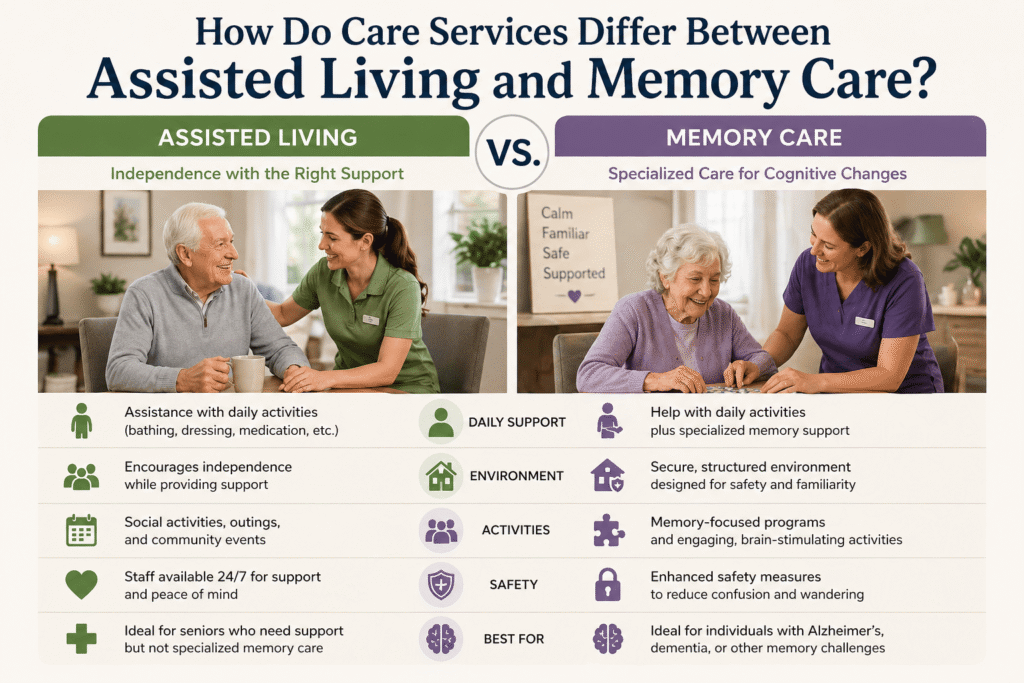

The difference between assisted living and memory care services centers on cognitive support versus physical assistance. Assisted living addresses mobility assistance and custodial care needs. Memory care provides comprehensive care including behavioral support, mental health services, and cognitive disorders management.
In assisted living with memory care programs, residents receive individualized support based on assessment processes. Care plans document specific needs and track progression. In contrast, standalone memory care offers dementia-specialized care with all programming designed for cognitive impairment assistance.
According to the American Seniors Housing Association (2024), staff ratios in memory care average 1:6 compared to 1:12 in assisted living. This enhanced supervision enables immediate response to wandering patients or behavioral episodes.
Daily Activity Differences
Assisted living daily activities emphasize social engagement through book clubs, fitness classes, and community outings. Residents participate based on personal preferences with minimal structured programming.
Memory care daily activities focus on cognitive stimulation through repetitive, simplified tasks. Programs accommodate early-stage dementia through late-stage dementia needs. Activities include sorting tasks, folding exercises, and music-based reminiscence reducing sundowning episodes.
What Are the Staffing and Training Differences?
Staff qualifications represent a critical distinction when comparing assisted living vs. memory care differences. Assisted living facilities employ certified nursing assistants with general geriatric care training. Memory care requires specialized dementia training covering Alzheimer’s disease progression, communication techniques for cognitive decline, and de-escalation strategies for behavioral changes.
According to the Alzheimer’s Association (2025), effective dementia care requires 16-24 hours of initial specialized training plus ongoing education. Memory care staff learn validation therapy, redirection techniques, and understanding neurological conditions affecting behavior.
Nursing staff composition differs significantly. Assisted living typically employs one registered nurse overseeing multiple licensed practical nurses. Memory care maintains higher nursing care ratios with on-site registered nurses during peak activity hours.
Professional Caregiving Requirements
- Assisted Living: Basic ADL assistance training, medication management certification, CPR/First Aid
- Memory Care: Dementia-specific modules, behavioral intervention protocols, memory support techniques, psychiatric care coordination
How Do Environmental Design and Safety Features Compare?
Environmental design in memory care neighborhoods incorporates dementia villages concepts with familiar settings reducing confusion. Color-coded hallways, pictorial signage, and circular floor plans enable safe wandering. Exit monitoring systems include delayed-egress locks and camouflaged exits preventing unsafe departures.
Assisted living floor plans resemble traditional apartments with private or semi-private rooms. Safety features focus on fall prevention through grab bars, emergency call systems, and well-lit pathways. Secure environment measures remain minimal as residents maintain freedom to leave independently.
According to research published in the Journal of the American Medical Directors Association (2024), environmental modifications in secured memory care reduce wandering incidents by 45% compared to general assisted living settings. Monitoring systems track resident location without restrictive interventions.
Security Measures Comparison
Memory Care Security:
- Keypad-controlled entry/exit points
- Visual monitoring throughout facility
- Enclosed outdoor courtyards
- GPS tracking technology for residents
- Staff positioned at strategic locations
Assisted Living Security:
- Front desk check-in systems
- Emergency response buttons in units
- General building security
- Wellness checks as scheduled
What Is the Cost Difference Between Assisted Living and Memory Care?
Memory care costs 20-50% more than assisted living due to enhanced staffing, specialized training, and secure facilities. According to Genworth’s Cost of Care Survey (2024), median monthly costs are $4,900 for assisted living versus $6,935 for memory care nationwide.
Private insurance rarely covers long-term care expenses. Medicare provides minimal coverage limited to skilled nursing facility stays following hospitalization. Medicaid covers eligible individuals in participating facilities, though memory care Medicaid acceptance varies by state.
Additional cost factors include medication management complexity, therapy services (physical therapy, occupational therapy, speech therapy), and level of supervision requirements. Some facilities offer tiered care systems with graduated care pricing as dementia progresses.
2025 National Average Monthly Costs
| Care Type | National Average | High-Cost Regions | Low-Cost Regions |
|---|---|---|---|
| Assisted Living | $4,900 | $7,500-$9,000 | $3,200-$4,200 |
| Memory Care | $6,935 | $9,500-$12,000 | $5,000-$6,200 |
| Skilled Nursing | $8,821 | $12,000-$15,000 | $6,500-$7,800 |
What Are the Eligibility and Assessment Requirements?
Assisted living admission criteria typically require needing assistance with two or more Activities of Daily Living (bathing, dressing, toileting, transferring, eating, continence). The assessment process evaluates physical capabilities, medication needs, and general health monitoring requirements.
Memory care admission criteria mandate documented cognitive impairment through physician diagnosis. Facilities assess mild cognitive impairment progression, dementia stages, and behavioral support needs. Some memory care facilities specialize in specific conditions like Alzheimer’s facilities or Parkinson’s disease programs.
According to the National Institute on Aging (2024), standardized cognitive assessments (Mini-Mental State Examination, Montreal Cognitive Assessment) determine appropriate care levels. Transition services help families understand when to move from assisted living to memory care as cognitive decline accelerates.
Transition Indicators: When to Switch from Assisted Living to Memory Care
- Frequent wandering episodes or getting lost in familiar areas
- Inability to recognize staff or family members consistently
- Aggressive behavioral changes or sundowning episodes
- Medication management becomes unsafe without supervision
- Declining participation in assisted living activities
- Safety concerns from confusion or poor judgment
- Progressive neurological conditions requiring specialized care
Real-World Scenarios: Which Option Fits Your Situation?
Scenario 1: Early-Stage Alzheimer’s with Mobility Independence
Background: Mary, 78, diagnosed with early-stage dementia, manages daily tasks but experiences memory problems and occasional confusion.
Recommendation: Assisted living with memory care programming. Mary benefits from social activities and personal assistance while accessing dementia education and monitoring systems as her condition progresses. The continuum of care allows seamless transition to dedicated memory care neighborhoods.
Scenario 2: Moderate Dementia with Wandering Behavior
Background: Robert, 82, has moderate dementia with frequent wandering attempts and sundowning episodes requiring around-the-clock supervision.
Recommendation: Standalone memory care. Robert requires secured memory care with exit monitoring, specialized dementia training staff, and structured environment preventing unsafe wandering. Behavioral support programs address sundowning through therapeutic activities and routine.
Scenario 3: Physical Limitations Without Cognitive Decline
Background: Patricia, 75, uses a walker, needs bathing assistance and meal preparation, but maintains mental sharpness.
Recommendation: Traditional assisted living. Patricia needs custodial care for physical limitations but benefits from independent living aspects. Assisted living communities provide mobility assistance, personal care services, and social engagement without cognitive restrictions.
Scenario 4: Vascular Dementia with Medical Complexity
Background: James, 80, has vascular dementia plus diabetes and heart conditions requiring frequent health monitoring and complex medication administration.
Recommendation: Memory care with enhanced medical support or skilled nursing facility. James needs both dementia-specific care and comprehensive medical oversight. Some memory care units offer nursing care sufficient for his needs; otherwise, nursing home alternatives provide necessary healthcare services.
Decision Framework: Choose Assisted Living If… / Choose Memory Care If…
Choose Assisted Living If:
- Your loved one needs help with 2-4 ADLs but remains cognitively intact
- They can follow directions and participate in group activities independently
- Safety concerns involve physical fall prevention rather than confusion-related risks
- They value independence and would feel restricted in locked units
- Budget constraints require lower-cost senior living options
- Socialization with cognitively healthy peers is important
- Medication management requires reminders but not constant supervision
Choose Memory Care If:
- Documented diagnosis of Alzheimer’s disease, dementia, or significant cognitive impairment
- Wandering behavior poses safety risks
- Behavioral changes require specialized dementia training to manage
- Confusion increases during evening hours (sundowning)
- Family caregiver burnout occurs from 24-hour supervision needs
- Standard assisted living lacks adequate cognitive support services
- Progression to moderate or severe dementia is occurring
- Psychiatric care or mental health services are regularly needed
Frequently Asked Questions About Assisted Living vs Memory Care
Can You Transition from Assisted Living to Memory Care in the Same Facility?
Yes. Many senior care facilities offer both levels within their continuum of care. Transition services facilitate moves between care levels as needs change. According to industry data (2024), approximately 65% of assisted living communities with memory care offer internal transfers, avoiding disruptive relocations.
Is Memory Care More Expensive Than Assisted Living?
Yes. Memory care typically costs 20-50% more due to specialized caregivers, lower staff ratios, enhanced safety features, and dementia-specific programming. Average additional costs range from $1,500-$3,000 monthly depending on region and facility amenities.
What Makes Memory Care Different from Assisted Living?
The primary difference involves specialized dementia care versus general elder care services. Memory care provides secured environments, staff with dementia training, therapeutic activities for cognitive disorders, and person-centered care addressing neurological conditions. Assisted living offers supportive living for physical needs without cognitive-specific programming.
How Do I Know When Someone Needs Memory Care Instead of Assisted Living?
Key indicators include: diagnosed cognitive impairment requiring specialized training, wandering prevention needs, behavioral support beyond general care capabilities, safety concerns from confusion, and care planning specifically for dementia stages. Professional assessment processes determine appropriate placement through standardized cognitive testing and care plan evaluation.